Chapters
Dec 03, 2025 // 20 min read
The Use of Tissue Level Design Implants in Immediate Protocols


Abstract
The tissue level (TL) implant is considered a challenging implant for the esthetic zone as the perceived potential esthetic risk of exposure of the machined collar or metal shine-through commonly drives clinicians to select bone level (BL) design implants, especially for immediate implant placement (IIP) protocols. Despite using BL design implants, studies investigating the outcomes of IIP have reported a high frequency of facial mucosal recession. In our experience, TL design implants provide comparable outcomes and seem to have been unfairly implicated for esthetic failures.
This article provides a narrative review of the evolution of TL implants and outlines the benefits of this design for IIP. Additionally, clinical cases are utilized to highlight the effectiveness of TL implants for IIP in the esthetic zone.
Based on the current evidence, there is a paucity of studies assessing the stability of clinical outcomes for IIP with TL implants in the esthetic zone. The standard indications and contra-indications apply regardless of implant type, and the optimal restoratively driven three-dimensional position of the implant should not be compromised.
Introduction
The tissue level (TL) implant has been at the forefront of innovation for more than four decades and is one of the oldest and most well-evidenced implants used in modern dentistry. At a time when Brånemark implants followed a fully submerged healing protocol, the one-piece TL (ITI) implants were novel, pushing the boundaries to pioneer transmucosal healing (Brånemark et al. 1969; Buser et al. 1990; Buser et al. 1997; Andersen et al. 2002).
As time progressed, surgical protocols were refined to allow for earlier placement and predictable loading protocols. Over the last two decades, the demands and benefits of immediate implant placement (IIP) have continued to increase from a patient and clinician perspective (den Hartog et al. 2008; Slagter et al. 2014; Huynh-Ba et al. 2018; Morton et al., 2018; Morton et al., 2023). IIP is defined as the placement of a dental implant into a fresh socket on the same day as tooth extraction (Gallucci et al. 2018).
Many readers might find it surprising that several early studies on IIP in the esthetic zone utilized TL implants as this was what was largely available at the time (Lang et al. 1994; Bragger et al. 1996; Andersen et al. 2002; Bianchi & Sanfilippo 2004). In the 1990s, these implants were parallel-sided with passive thread designs and, with developing IIP protocols, were considered technically demanding to place and lacked sufficient primary stability for IIP. From 2000 onwards, bone level (BL) design implants gained preference and have been predominantly used in research studies, with the introduction of implant geometries that offer relatively predictable high primary stability at implant insertion (Cochran et al. 2016; Dard et al. 2016). Until recently, implant geometries that aid immediate protocols have been largely absent from manufacturer portfolios for TL implants, and therefore, modern studies have rarely reported outcomes of TL implants (Wittneben et al. 2023). However, the authors believe TL implants can be successfully and predictably utilized for IIP in the anterior esthetic zone and achieve stable long-term esthetic outcomes.
It is to be reiterated that replacing a single tooth in the anterior maxilla (#15 to #25) with an IIP protocol is a complex procedure. The rules for placing TL immediate implants in the anterior maxillary esthetic zone are similar to those for BL design implants. IIP may be considered the treatment of choice when ideal conditions are present (Wittneben et al. 2023), such as:
- Healthy adjacent teeth
- Thick gingival phenotype
- Intact facial bone >1 mm in thickness
- No acute infection or chronic fistula
- Ability to place the implant in the correct three-dimensional position for a screw-retained restoration
- Ability to achieve primary stability of the implant, which is a fundamental prerequisite if an immediate restoration is expected.
This article aims to discuss the tissue level implant’s potential advantages, address concerns about its use, and highlight the esthetic outcomes achievable when immediately placing TL implants in the esthetic zone.
Caution with immediate implant placement
Immediate implants are associated with greater variability in esthetic outcomes with a higher frequency of facial mucosal recession of >1 mm compared to early implant placement (Chen and Buser 2014; Hamilton et al. 2023). Careful assessment and analysis are crucial for appropriately determining any treatment plan, especially when proposing IIP treatment in the esthetic zone (Wittneben et al. 2023). An ethos of “minimizing morbidity without compromising long-term outcomes” should be prioritized.
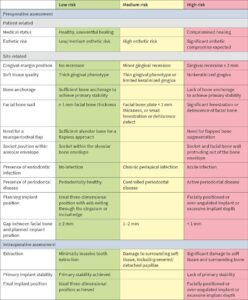
Patient and site-related factors must be considered for treatment to achieve predictable long-term functional and esthetic outcomes. The patient could be assessed using the Esthetic Risk Assessment (ERA) and risk assessment for IIP in single-tooth sites (Table 1) (Hamilton et al. 2023; Lambert et al. 2023) to determine the patient and site-specific risk factors for IIP. If the criteria for IIP protocol are not met, alternative placement protocols must be considered.
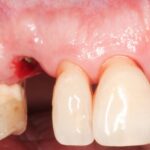
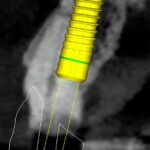
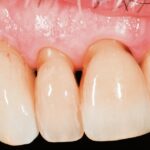
Optimizing esthetics for implant restorations in the anterior maxilla has been well studied, and implants should be restoratively driven irrespective of the timing of implant placement. It is critical to achieve an optimal, prosthetically-driven, three-dimensional implant position (Buser et al. 2004; Buser et al. 2017). In the anterior maxilla, midfacial recession has been reported for immediately placed BL implants in the presence of a thin (<1 mm) or missing facial bone plate (Chen et al. 2007; Seyssens et al. 2020). Further, clinical studies using CBCT scans to examine the facial bone on immediately placed implants have shown a significant relationship between recessions of the midfacial mucosa and a lack of visible facial bone on the CBCT images (Januário et al. 2011; Miyamoto & Obama 2011; Benic et al. 2012). The risks can be similar for TL implants, but the authors have experienced minimal risk of increased mucosal recession after placing TL implants in patients with <1 mm facial bone (Fig. 2). Although not currently supported by evidence, we attribute this to the simultaneous osseo- and mucosal integration that allows for better soft and hard tissue stability. Nevertheless, in some cases, loss of alveolar convexity has been noted, and the CBCT scans have confirmed the loss of alveolar convexity (Fig. 3).
After minimally traumatic extraction and preservation of facial bone plate, an immediate TL implant (NNC design) was placed (Type 1B) with simultaneous bone grafting in a 71-year-old male. The definitive restoration was placed 6 weeks later (Fig. 2c). For up to four years, the peri-implant tissues were stable with minimal recession, whilst there was a noticeable recession in adjoining natural teeth (Fig. 2d). There was minimal loss of alveolar contour despite <1 mm facial bone wall thickness (Fig. 2e). What is interesting to note here is that the bone is detectable coronal to the rough-smooth transition (Fig. 2f), which is not uncommon in our experience. Although histologically, this bone will not be “osseointegrated” with the machined collar, this thick, stable architecture achieved by the TL likely contributes to the long-term stable esthetics seen in our experience with TL implants.
In Figs 3a – c, a 75-year-old male requiring replacement of UL2 also has <1 mm facial bone thickness and pre-existing recession and a peri-apical lesion. Similar to the previous case, a Type 1B protocol with simultaneous GBR was chosen (Fig. 3d) (Gallucci et al. 2018). Loss of alveolar convexity was noted within weeks of provisionalization, even though the submarginal emergence of the crown was optimally shaped (Figs 3e – g). Nevertheless, the 1- and 2-year reviews show an excellent esthetic outcome (Figs 3h – k), which compares well with the pre-operative situation.
These two examples reiterate that outcomes with Type 1 protocols, especially the response of bundle bone resorption and its impact on bone graft particles, can be unpredictable, even with TL implants.
Interestingly, pre-clinical studies have consistently demonstrated that irrespective of implant type or dimension, resorption of bone after tooth extraction occurs (Araujo & Lindhe 2005; Caneva et al. 2010; Linares et al. 2011). Caneva and coworkers highlighted the need for sufficient space between the implant and the buccal bone. They studied the influence of the distance of the implant surface to the buccal bone for IIP by comparing 3.3-mm and 5-mm diameter implants. Marginal bone loss in wider diameter implants was more marked compared to the narrow diameter implants. This risk is heightened in thin phenotypes, so coronally tapered implants such as the Straumann TE are now not commonly used for IIP. Therefore, IIP in sites with a facial bone thickness of <1 mm should be considered a risk for loss of alveolar root convexity and midfacial recession. In such cases, if IIP is preferred, soft tissue augmentation at the time of placement should be considered (Seyssens et al. 2021).
One of the main concerns regarding TL in the esthetic zone is the risk of shine-through or exposure of the machined collar. In our experience, these complications result solely from surgical error and due to facial malpositioning of the implant (Chen et al. 2007; Chen et al. 2009), resulting in recession and esthetic failure (Chen & Buser 2009; Cosyn et al. 2019; Evans & Chen 2008). Most importantly, these complications arise irrespective of the chosen implant design.
Tissue level implants in the Type 1 immediate protocol should be placed, adhering to the principles of 3-dimensional implant placement (Figs 4 – 5):
Apico-coronal position: not more than 2-3 mm apical to the proposed mucosal margin,
- Oro-facial position: ideally screw-retained with screw access through the cingulum. A minimum of 2-mm horizontal gap should be maintained between implant and internal socket wall at the junction of the rough surface,
- Mesio-distal position: >1.5 mm distance from implant shoulder to adjacent teeth.
References
Abrahamsson I, Berglundh T, Lindhe J. The mucosal barrier following abutment dis/reconnection. An experimental study in dogs. J Clin Periodontol. 1997 Aug;24(8):568-72. doi: 10.1111/j.1600-051x.1997.tb00230.x. PMID: 9266344.
Akkocaoglu M, Uysal S, Tekdemir I, Akca K, Cehreli MC. Implant design and intraosseous stability of immediately placed implants: a human cadaver study. Clin Oral Implants Res. 2005 Apr;16(2):202-9. doi: 10.1111/j.1600-0501.2004.01099.x. PMID: 15777330.
Alves CC, Muñoz F, Cantalapiedra A, Ramos I, Neves M, Blanco J. Marginal bone and soft tissue behavior following platform switching abutment connection/disconnection–a dog model study. Clin Oral Implants Res. 2015 Sep;26(9):983-91. doi: 10.1111/clr.12385. Epub 2014 Apr 16. PMID: 24735458.
Andersen E, Haanaes HR, Knutsen BM. Immediate loading of single-tooth ITI implants in the anterior maxilla: a prospective 5-year pilot study. Clin Oral Implants Res. 2002 Jun;13(3):281-7. doi: 10.1034/j.1600-0501.2002.130307.x. PMID: 12010158.
Araújo MG, Lindhe J. Dimensional ridge alterations following tooth extraction. An experimental study in the dog. J Clin Periodontol. 2005 Feb;32(2):212-8. doi: 10.1111/j.1600-051X.2005.00642.x. PMID: 15691354.
Atieh MA, Ibrahim HM, Atieh AH. Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. J Periodontol. 2010 Oct;81(10):1350-66. doi: 10.1902/jop.2010.100232. PMID: 20575657.
Benic GI, Mokti M, Chen CJ, Weber HP, Hämmerle CH, Gallucci GO. Dimensions of buccal bone and mucosa at immediately placed implants after 7 years: a clinical and cone beam computed tomography study. Clin Oral Implants Res. 2012 May;23(5):560-6. doi: 10.1111/j.1600-0501.2011.02253.x. Epub 2011 Sep 8. PMID: 22093013.
Berglundh T, Lindhe J. Dimension of the periimplant mucosa. Biological width revisited. J Clin Periodontol. 1996 Oct;23(10):971-3. doi: 10.1111/j.1600-051x.1996.tb00520.x. PMID: 8915028.
Bianchi AE, Sanfilippo F. Single-tooth replacement by immediate implant and connective tissue graft: a 1-9-year clinical evaluation. Clin Oral Implants Res. 2004 Jun;15(3):269-77. doi: 10.1111/j.1600-0501.2004.01020.x. PMID: 15142088.
Brägger U, Hämmerle CH, Lang NP. Immediate transmucosal implants using the principle of guided tissue regeneration (II). A cross-sectional study comparing the clinical outcome 1 year after immediate to standard implant placement. Clin Oral Implants Res. 1996 Sep;7(3):268-76. doi: 10.1034/j.1600-0501.1996.070309.x. PMID: 9151591.
Brånemark PI, Adell R, Breine U, Hansson BO, Lindström J, Ohlsson A. Intra-osseous anchorage of dental prostheses. I. Experimental studies. Scand J Plast Reconstr Surg. 1969;3(2):81-100. doi: 10.3109/02844316909036699. PMID: 4924041.
Bressan E, Guazzo R, Tomasi C, Peña TG, Galindo-Moreno P, Caponio VCA, Sbricoli L, Canullo L. Influence of soft tissue thickness on marginal bone level around dental implants: A systematic review with meta-analysis and trial-sequential analysis. Clin Oral Implants Res. 2023 May;34(5):405-415. doi: 10.1111/clr.14032. Epub 2023 Mar 13. PMID: 36737243.
Broggini N, McManus LM, Hermann JS, Medina RU, Oates TW, Schenk RK, Buser D, Mellonig JT, Cochran DL. Persistent acute inflammation at the implant-abutment interface. J Dent Res. 2003 Mar;82(3):232-7. doi: 10.1177/154405910308200316. PMID: 12598555.
Buser D, Chappuis V, Belser UC, Chen S. Implant placement post extraction in esthetic single tooth sites: when immediate, when early, when late? Periodontol 2000. 2017 Feb;73(1):84-102. doi: 10.1111/prd.12170. PMID: 28000278.
Buser D, Chappuis V, Bornstein MM, Wittneben JG, Frei M, Belser UC. Long-term stability of contour augmentation with early implant placement following single tooth extraction in the esthetic zone: a prospective, cross-sectional study in 41 patients with a 5- to 9-year follow-up. J Periodontol. 2013 Nov;84(11):1517-27. doi: 10.1902/jop.2013.120635. Epub 2013 Jan 24. PMID: 23347346.
Buser D, Martin W, Belser UC. Optimizing esthetics for implant restorations in the anterior maxilla: anatomic and surgical considerations. Int J Oral Maxillofac Implants. 2004;19 Suppl:43-61. PMID: 15635945.
Buser D, Mericske-Stern R, Bernard JP, Behneke A, Behneke N, Hirt HP, Belser UC, Lang NP. Long-term evaluation of non-submerged ITI implants. Part 1: 8-year life table analysis of a prospective multi-center study with 2359 implants. Clin Oral Implants Res. 1997 Jun;8(3):161-72. doi: 10.1034/j.1600-0501.1997.080302.x. PMID: 9586460.
Buser D, Weber HP, Lang NP. Tissue integration of non-submerged implants. 1-year results of a prospective study with 100 ITI hollow-cylinder and hollow-screw implants. Clin Oral Implants Res. 1990 Dec;1(1):33-40. doi: 10.1034/j.1600-0501.1990.010105.x. PMID: 2099210.
Chappuis V, Bornstein MM, Buser D, Belser U. Influence of implant neck design on facial bone crest dimensions in the esthetic zone analyzed by cone beam CT: a comparative study with a 5-to-9-year follow-up. Clin Oral Implants Res. 2016 Sep;27(9):1055-64. doi: 10.1111/clr.12692. Epub 2015 Sep 15. PMID: 26370904.
Chen ST, Buser D. Esthetic outcomes following immediate and early implant placement in the anterior maxilla–a systematic review. Int J Oral Maxillofac Implants. 2014;29 Suppl:186-215. doi: 10.11607/jomi.2014suppl.g3.3. PMID: 24660198.
Calatrava J, Sanz-Sánchez I, Molina A, Bollain J, Martín C, Sanz M. Effect of one-time placement of the definitive abutment versus multiple healing abutment disconnections and reconnections during the prosthetic phase on radiographic and clinical outcomes: A 12-month randomized clinical trial. Clin Implant Dent Relat Res. 2024 Oct;26(5):998-1011. doi: 10.1111/cid.13361. Epub 2024 Jul 16. PMID: 39011816.
Canullo L, Fedele GR, Iannello G, Jepsen S. Platform switching and marginal bone-level alterations: the results of a randomized-controlled trial. Clin Oral Implants Res. 2010 Jan;21(1):115-21. doi: 10.1111/j.1600-0501.2009.01867.x. PMID: 20070752.
Caneva M, Salata LA, de Souza SS, Bressan E, Botticelli D, Lang NP. Hard tissue formation adjacent to implants of various size and configuration immediately placed into extraction sockets: an experimental study in dogs. Clin Oral Implants Res. 2010 Sep;21(9):885-90. doi: 10.1111/j.1600-0501.2010.01931.x. Epub 2010 May 9. PMID: 20491839.
Canullo L, Goglia G, Iurlaro G, Iannello G. Short-term bone level observations associated with platform switching in immediately placed and restored single maxillary implants: a preliminary report. Int J Prosthodont. 2009 May-Jun;22(3):277-82. PMID: 19548410.
Chen ST, Buser D. Clinical and esthetic outcomes of implants placed in postextraction sites. Int J Oral Maxillofac Implants. 2009;24 Suppl:186-217. PMID: 19885446.
Chen ST, Darby IB, Reynolds EC. A prospective clinical study of non-submerged immediate implants: clinical outcomes and esthetic results. Clin Oral Implants Res. 2007 Oct;18(5):552-62. doi: 10.1111/j.1600-0501.2007.01388.x. Epub 2007 Jun 30. PMID: 17608739.
Chen ST, Darby IB, Reynolds EC, Clement JG. Immediate implant placement postextraction without flap elevation. J Periodontol. 2009 Jan;80(1):163-72. doi: 10.1902/jop.2009.080243. PMID: 19228102.
Cochran D, Stavropoulos A, Obrecht M, Pippenger B, Dard M. A Comparison of Tapered and Nontapered Implants in the Minipig. Int J Oral Maxillofac Implants. 2016 Nov/Dec;31(6):1341-1347. doi: 10.11607/jomi.4712. PMID: 27861658.
Cosyn J, De Lat L, Seyssens L, Doornewaard R, Deschepper E, Vervaeke S. The effectiveness of immediate implant placement for single tooth replacement compared to delayed implant placement: A systematic review and meta-analysis. J Clin Periodontol. 2019 Jun;46 Suppl 21:224-241. doi: 10.1111/jcpe.13054. PMID: 30624808.
Dard M, Kuehne S, Obrecht M, Grandin M, Helfenstein J, Pippenger BE. Integrative Performance Analysis of a Novel Bone Level Tapered Implant. Adv Dent Res. 2016 Mar;28(1):28-33. doi: 10.1177/0022034515624443. PMID: 26927485.
De Sanctis M, Vignoletti F, Discepoli N, Muñoz F, Sanz M. Immediate implants at fresh extraction sockets: an experimental study in the beagle dog comparing four different implant systems. Soft tissue findings. J Clin Periodontol. 2010 Aug 1;37(8):769-76. doi: 10.1111/j.1600-051X.2010.01570.x. Epub 2010 Jun 1. PMID: 20528965.
den Hartog L, Slater JJ, Vissink A, Meijer HJ, Raghoebar GM. Treatment outcome of immediate, early and conventional single-tooth implants in the aesthetic zone: a systematic review to survival, bone level, soft-tissue, aesthetics and patient satisfaction. J Clin Periodontol. 2008 Dec;35(12):1073-86. doi: 10.1111/j.1600-051X.2008.01330.x. PMID: 19040585.
Derks J, Schaller D, Håkansson J, Wennström JL, Tomasi C, Berglundh T. Peri-implantitis – onset and pattern of progression. J Clin Periodontol. 2016 Apr;43(4):383-8. doi: 10.1111/jcpe.12535. Epub 2016 Mar 29. PMID: 26900869.
El Chaar E, Puisys A, Sabbag I, Bellón B, Georgantza A, Kye W, Pippenger BE. A novel fully tapered, self-cutting tissue-level implant: non-inferiority study in minipigs. Clin Oral Investig. 2021 Nov;25(11):6127-6137. doi: 10.1007/s00784-021-03912-w. Epub 2021 Apr 16. PMID: 33861379; PMCID: PMC8531107.
Ellis R, Chen S, Davies H, Fitzgerald W, Xu J, Darby I. Primary stability and healing outcomes of apically tapered and straight implants placed into fresh extraction sockets. A pre-clinical in vivo study. Clin Oral Implants Res. 2020 Aug;31(8):705-714. doi: 10.1111/clr.13618. Epub 2020 Jun 17. PMID: 32455469.
Evans CD, Chen ST. Esthetic outcomes of immediate implant placements. Clin Oral Implants Res. 2008 Jan;19(1):73-80. doi: 10.1111/j.1600-0501.2007.01413.x. Epub 2007 Oct 22. PMID: 17956569.
Gallucci GO, Hamilton A, Zhou W, Buser D, Chen S. Implant placement and loading protocols in partially edentulous patients: A systematic review. Clin Oral Implants Res. 2018 Oct;29 Suppl 16:106-134. doi: 10.1111/clr.13276. PMID: 30328194.
Gill T, Kühl S, Rawlinson S, Pippenger B, Bellon B, Shahdad S. Primary stability and osseointegration comparing a novel tapered design tissue-level implant with a parallel design tissue-level implant. An experimental in vivo study. Clin Oral Implants Res. 2024 Sep;35(9):1114-1127. doi: 10.1111/clr.14301. Epub 2024 May 31. PMID: 38819108.
Hamilton A, Gonzaga L, Amorim K, Wittneben JG, Martig L, Morton D, Martin W, Gallucci GO, Wismeijer D. Selection criteria for immediate implant placement and immediate loading for single tooth replacement in the maxillary esthetic zone: A systematic review and meta-analysis. Clin Oral Implants Res. 2023 Sep;34 Suppl 26:304-348. doi: 10.1111/clr.14109. PMID: 37750515.
Hänggi MP, Hänggi DC, Schoolfield JD, Meyer J, Cochran DL, Hermann JS. Crestal bone changes around titanium implants. Part I: A retrospective radiographic evaluation in humans comparing two non-submerged implant designs with different machined collar lengths. J Periodontol. 2005 May;76(5):791-802. doi: 10.1902/jop.2005.76.5.791. PMID: 15898941.
Hermann JS, Jones AA, Bakaeen LG, Buser D, Schoolfield JD, Cochran DL. Influence of a machined collar on crestal bone changes around titanium implants: a histometric study in the canine mandible. J Periodontol. 2011 Sep;82(9):1329-38. doi: 10.1902/jop.2011.090728. Epub 2011 Apr 12. PMID: 21486176.
Hermann JS, Schoolfield JD, Schenk RK, Buser D, Cochran DL. Influence of the size of the microgap on crestal bone changes around titanium implants. A histometric evaluation of unloaded non-submerged implants in the canine mandible. J Periodontol. 2001 Oct;72(10):1372-83. doi: 10.1902/jop.2001.72.10.1372. PMID: 11699479.
Huynh-Ba G, Oates TW, Williams MAH. Immediate loading vs. early/conventional loading of immediately placed implants in partially edentulous patients from the patients’ perspective: A systematic review. Clin Oral Implants Res. 2018 Oct;29 Suppl 16:255-269. doi: 10.1111/clr.13278. PMID: 30328205.
Javed F, Romanos GE. The role of primary stability for successful immediate loading of dental implants. A literature review. J Dent. 2010 Aug;38(8):612-20. doi: 10.1016/j.jdent.2010.05.013. Epub 2010 Jun 11. PMID: 20546821.
Januário AL, Duarte WR, Barriviera M, Mesti JC, Araújo MG, Lindhe J. Dimension of the facial bone wall in the anterior maxilla: a cone-beam computed tomography study. Clin Oral Implants Res. 2011 Oct;22(10):1168-1171. doi: 10.1111/j.1600-0501.2010.02086.x. Epub 2011 Feb 15. PMID: 21320168.
Kan JY, Rungcharassaeng K, Lozada J. Immediate placement and provisionalization of maxillary anterior single implants: 1-year prospective study. Int J Oral Maxillofac Implants. 2003 Jan-Feb;18(1):31-9. PMID: 12608666.
Kan JY, Roe P, Rungcharassaeng K, Patel RD, Waki T, Lozada JL, Zimmerman G. Classification of sagittal root position in relation to the anterior maxillary osseous housing for immediate implant placement: a cone beam computed tomography study. Int J Oral Maxillofac Implants. 2011 Jul-Aug;26(4):873-6. PMID: 21841998.
Kan JY, Rungcharassaeng K, Sclar A, Lozada JL. Effects of the facial osseous defect morphology on gingival dynamics after immediate tooth replacement and guided bone regeneration: 1-year results. J Oral Maxillofac Surg. 2007 Jul;65(7 Suppl 1):13-9. doi: 10.1016/j.joms.2007.04.006. Erratum in: J Oral Maxillofac Surg. 2008 Oct;66(10):2195-6. PMID: 17586345.
Kim S, Jung UW, Cho KS, Lee JS. Retrospective radiographic observational study of 1692 Straumann tissue-level dental implants over 10 years: I. Implant survival and loss pattern. Clin Implant Dent Relat Res. 2018 Oct;20(5):860-866. doi: 10.1111/cid.12659. Epub 2018 Aug 15. PMID: 30110515.
Lago L, da Silva L, Martinez-Silva I, Rilo B. Crestal Bone Level Around Tissue-Level Implants Restored with Platform Matching and Bone-Level Implants Restored with Platform Switching: A 5-Year Randomized Controlled Trial. Int J Oral Maxillofac Implants. 2018 Mar/Apr;33(2):448-456. doi: 10.11607/jomi.6149. PMID: 29534134.
Lambert, F., Hamilton, A., De Souza, A., & Martin, W. (2023). Pre-operative analysis and treatment planning. In D. Wismeijer, Bart, & N. Donos (Eds.), ITI treatment guide 14: Immediate implant placement and restoration in partially edentulous patients (Vol. 14). Quintessence.
Lang NP, Brägger U, Hämmerle CH, Sutter F. Immediate transmucosal implants using the principle of guided tissue regeneration. I. Rationale, clinical procedures and 30-month results. Clin Oral Implants Res. 1994 Sep;5(3):154-63. doi: 10.1034/j.1600-0501.1994.050306.x. PMID: 7827230.
Lazzara RJ, Porter SS. Platform switching: a new concept in implant dentistry for controlling postrestorative crestal bone levels. Int J Periodontics Restorative Dent. 2006 Feb;26(1):9-17. PMID: 16515092.
Liñares A, Mardas N, Dard M, Donos N. Effect of immediate or delayed loading following immediate placement of implants with a modified surface. Clin Oral Implants Res. 2011 Jan;22(1):38-46. doi: 10.1111/j.1600-0501.2010.01988.x. Epub 2010 Oct 6. PMID: 21039892.
Liu Y, Wang J. Influences of microgap and micromotion of implant-abutment interface on marginal bone loss around implant neck. Arch Oral Biol. 2017 Nov;83:153-160. doi: 10.1016/j.archoralbio.2017.07.022. Epub 2017 Jul 29. PMID: 28780384.
Maeda Y, Miura J, Taki I, Sogo M. Biomechanical analysis on platform switching: is there any biomechanical rationale? Clin Oral Implants Res. 2007 Oct;18(5):581-4. doi: 10.1111/j.1600-0501.2007.01398.x. Epub 2007 Jun 30. PMID: 17608737.
Miyamoto Y, Obama T. Dental cone beam computed tomography analyses of postoperative labial bone thickness in maxillary anterior implants: comparing immediate and delayed implant placement. Int J Periodontics Restorative Dent. 2011 Jun;31(3):215-25. PMID: 21556378.
Molina A, Sanz-Sánchez I, Martín C, Blanco J, Sanz M. The effect of one-time abutment placement on interproximal bone levels and peri-implant soft tissues: a prospective randomized clinical trial. Clin Oral Implants Res. 2017 Apr;28(4):443-452. doi: 10.1111/clr.12818. Epub 2016 Mar 25. PMID: 27016157.
Morton D, Gallucci G, Lin WS, Pjetursson B, Polido W, Roehling S, Sailer I, Aghaloo T, Albera H, Bohner L, Braut V, Buser D, Chen S, Dawson A, Eckert S, Gahlert M, Hamilton A, Jaffin R, Jarry C, Karayazgan B, Laine J, Martin W, Rahman L, Schlegel A, Shiota M, Stilwell C, Vorster C, Zembic A, Zhou W. Group 2 ITI Consensus Report: Prosthodontics and implant dentistry. Clin Oral Implants Res. 2018 Oct;29 Suppl 16:215-223. doi: 10.1111/clr.13298. PMID: 30328196.
Morton D, Wismeijer D, Chen S, Hamilton A, Wittneben J, Casentini P, Gonzaga L, Lazarin R, Martin W, Molinero-Mourelle P, Obermailer B, Polido WD, Tahmaseb A, Thoma D, Zembic A. Group 5 ITI Consensus Report: Implant placement and loading protocols. Clin Oral Implants Res. 2023 Sep;34 Suppl 26:349-356. doi: 10.1111/clr.14137. PMID: 37750529.
Oskarsson M, Otsuki M, Welander M, Abrahamsson I. Peri-implant tissue healing at implants with different designs and placement protocols: An experimental study in dogs. Clin Oral Implants Res. 2018 Aug;29(8):873-880. doi: 10.1111/clr.13339. Epub 2018 Jul 16. PMID: 30009476.
Parvini P, Buser D, Pippenger BE, Imber JC, Stavropoulos A, Bellón B, Jarry C, Schwarz F. Influence of loading and grafting on hard- and soft-tissue healing at immediately placed implants: An experimental study in minipigs. J Clin Periodontol. 2023 Feb;50(2):232-241. doi: 10.1111/jcpe.13734. Epub 2022 Oct 19. PMID: 36217692; PMCID: PMC10092114.
Quah B, Al Yousef AS, Lai CWM, Wong RCW, Chew RJJ. Impact of Implant Design on Outcomes of Simultaneous Guided Bone Regeneration for Dehiscence Defects: A Systematic Review and Meta-Analysis. J Evid Based Dent Pract. 2024 Dec;24(4):102033. doi: 10.1016/j.jebdp.2024.102033. Epub 2024 Aug 16. PMID: 39631971.
Rathi PR, Kolte RA, Kolte AP. Comparative evaluation of peri-implant tissues in definitive and repeated abutment replacements: A randomized clinical trial. J Indian Soc Periodontol. 2022 Jan-Feb;26(1):44-50. doi: 10.4103/jisp.jisp_335_20. Epub 2022 Jan 1. PMID: 35136316; PMCID: PMC8796786.
Roccuzzo M, Wilson TG Jr, Ucer C, Beagle JR. Immediate placement of tapered effect (TE) implants: 5-year results of a prospective, multicenter study. Int J Oral Maxillofac Implants. 2013;28(1):261-269. doi:10.11607/jomi.2678.
Romandini M, Pedrinaci I, Lima C, Soldini MC, Araoz A, Sanz M. Prevalence and risk/protective indicators of buccal soft tissue dehiscence around dental implants. J Clin Periodontol. 2021 Mar;48(3):455-463. doi: 10.1111/jcpe.13417. Epub 2021 Jan 21. PMID: 33378079.
Salvi GE, Bosshardt DD, Lang NP, Abrahamsson I, Berglundh T, Lindhe J, Ivanovski S, Donos N. Temporal sequence of hard and soft tissue healing around titanium dental implants. Periodontol 2000. 2015 Jun;68(1):135-52. doi: 10.1111/prd.12054. PMID: 25867984.
Sanz-Sánchez I, Molina A, Martin C, Bollain J, Calatrava J, Sanz M. The effect of one-time abutment placement on clinical and radiographic outcomes: A 5-year randomized clinical trial. Clin Oral Implants Res. 2024 Jun;35(6):609-620. doi: 10.1111/clr.14256. Epub 2024 Mar 20. PMID: 38506392.
Sasada Y, Cochran DL. Implant-Abutment Connections: A Review of Biologic Consequences and Peri-implantitis Implications. Int J Oral Maxillofac Implants. 2017 Nov/Dec;32(6):1296-1307. doi: 10.11607/jomi.5732. PMID: 29140374.
Schiegnitz E, Sagheb K, Raahimi L, König J, Azaripour A, Al-Nawas B. Immediate versus delayed implant placement of novel fully tapered tissue-level implants – A retrospective multicenter clinical study. Clin Oral Implants Res. 2024 Jun;35(6):668-676. doi: 10.1111/clr.14263. Epub 2024 Apr 4. PMID: 38572982.
Seyssens L, De Lat L, Cosyn J. Immediate implant placement with or without connective tissue graft: A systematic review and meta-analysis. J Clin Periodontol. 2021 Feb;48(2):284-301. doi: 10.1111/jcpe.13397. Epub 2020 Nov 20. PMID: 33125754.
Seyssens L, Eghbali A, Cosyn J. A 10-year prospective study on single immediate implants. J Clin Periodontol. 2020 Oct;47(10):1248-1258. doi: 10.1111/jcpe.13352. Epub 2020 Sep 2. PMID: 32748983.
Shahdad SA, Apostoulous I, Lynch E, Gamboa A, Taylor P, Pawar R, Makdissi J. Investigation to determine the aesthetic outcome of implant restorations in maxillary aesthetic zone and its relationship to the labial bone thickness using clinical evaluation and dental computed tomography (CBCT) scanning technique. IPJ Dent & Oral Med 2013; 3:653
Shahdad S, Makdissi J, Gambôa A. Relationship Between Facial Bone Dimensions, Orofacial Implant Position, and Esthetic Outcomes of Single-Tooth Implants. Int J Prosthodont. 2023 Dec 18;36(6):668-673. doi: 10.11607/ijp.8052. PMID: 38109386.
Slagter KW, den Hartog L, Bakker NA, Vissink A, Meijer HJ, Raghoebar GM. Immediate placement of dental implants in the esthetic zone: a systematic review and pooled analysis. J Periodontol. 2014 Jul;85(7):e241-50. doi: 10.1902/jop.2014.130632. Epub 2014 Feb 6. PMID: 24502614.
Strietzel FP, Neumann K, Hertel M. Impact of platform switching on marginal peri-implant bone-level changes. A systematic review and meta-analysis. Clin Oral Implants Res. 2015 Mar;26(3):342-58. doi: 10.1111/clr.12339. Epub 2014 Jan 20. PMID: 24438506; PMCID: PMC4340042.
Tavelli L, Barootchi S, Avila-Ortiz G, Urban IA, Giannobile WV, Wang HL. Peri-implant soft tissue phenotype modification and its impact on peri-implant health: A systematic review and network meta-analysis. J Periodontol. 2021 Jan;92(1):21-44. doi: 10.1002/JPER.19-0716. Epub 2020 Aug 9. PMID: 32710810.
Tomar S, Saxena D, Kaur N. Marginal bone loss around implants with platform switching and platform matched connection: A systematic review. J Prosthet Dent. 2023 Oct 18:S0022-3913(23)00622-4. doi: 10.1016/j.prosdent.2023.09.009. Epub ahead of print. PMID: 37863757.
Wilson TG Jr, Roccuzzo M, Ucer C, Beagle JR. Immediate placement of tapered effect (TE) implants: 5-year results of a prospective, multicenter study. Int J Oral Maxillofac Implants. 2013 Jan-Feb;28(1):261-9. doi: 10.11607/jomi.2678. PMID: 23377073.
Wittneben JG, Molinero-Mourelle P, Hamilton A, Alnasser M, Obermaier B, Morton D, Gallucci GO, Wismeijer D. Clinical performance of immediately placed and immediately loaded single implants in the esthetic zone: A systematic review and meta-analysis. Clin Oral Implants Res. 2023 Sep;34 Suppl 26:266-303. doi: 10.1111/clr.14172. PMID: 37750531.